Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Topic Contents
Gastroesophageal Reflux in Babies and Children
Condition Basics
What is gastroesophageal reflux in babies and children?
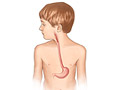
Gastroesophageal reflux is a backflow (reflux or regurgitation) of food and stomach acid into the esophagus. This is the tube that connects the throat to the stomach. When reflux irritates the lining of the esophagus and causes burning pain, difficulty eating, weight loss, or other problems, it is called gastroesophageal reflux disease (GERD).
Reflux is common in babies and children. It's most often not a sign of a serious problem. Most babies stop having reflux around 1 year of age. A child who continues to have reflux may need treatment.
What causes it?
Gastroesophageal reflux happens because of a problem with the ring of muscle at the end of the esophagus. The ring of muscle is called the lower esophageal sphincter. It acts like a one-way valve between the esophagus and the stomach. When your child swallows, the valve lets food pass into the stomach. If the valve is weak, stomach contents can flow back up into the esophagus.
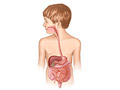
In babies, this problem happens because the digestive tract is still growing. Reflux usually goes away as a baby matures.
What are the symptoms?
It is common for babies to spit up (have reflux) after they eat. Babies with severe gastroesophageal reflux may cry, act fussy, or have trouble eating. They may not sleep well or grow as expected.
An older child or teen may have the same symptoms as an adult. They may cough a lot and have a burning feeling in the chest and throat (heartburn). They may have a sour or bitter taste in the mouth.
If stomach acid goes up to the throat or into the airways, a child may get hoarse or have a lasting cough. Reflux can also cause pneumonia or wheezing, and it may hurt to swallow.
How is it diagnosed?
Gastroesophageal reflux is a backflow (reflux or regurgitation) of food and stomach acid into the esophagus, which is the tube that connects the throat to the stomach. To find out if a child has gastroesophageal reflux, a doctor will do a physical exam and ask about symptoms.
Tests are not usually needed. But sometimes they are recommended when your doctor is worried that something other than gastroesophageal reflux is causing symptoms. Or they might be needed if your child has other symptoms like coughing. Tests can include:
- A barium swallow. This is a series of X-rays that shows the esophagus and stomach.
- Endoscopy. This lets the doctor look at the esophagus.
- An esophageal pH test. This measures how much acid is in the esophagus.
How is gastroesophageal reflux treated in babies and children?
Most babies stop having gastroesophageal reflux over time, so the doctor may just suggest that you follow some steps to help reduce the problem until it goes away. For example, it may help to:
- Burp your baby a few times during each feeding.
- Keep your baby upright for 30 minutes after each feeding. Avoid a "car seat position," because sitting can make reflux worse in babies.
- Avoid feeding too much at one time. Give your baby smaller meals more often.
- Thicken your baby's formula with a small amount of rice cereal if your doctor recommends it.
- Keep your baby away from smoky areas.
For older children and teens, it may help to:
- Avoid large meals before exercise.
- Raise the head of your child's bed a little bit. Using extra pillows does not work. Do not raise the head of your child's bed if your child is younger than 12 months.
- Have your child wait 2 to 3 hours before they lie down. Snacking close to bedtime can make their symptoms worse.
- Serve 5 or 6 small meals instead of 2 or 3 large meals.
- Avoid foods that make your child's symptoms worse. These may include chocolate, mint, alcohol, pepper, spicy foods, high-fat foods, or drinks with caffeine in them, such as tea, coffee, colas, or energy drinks. If your child's symptoms are worse after they eat a certain food, they can stop eating it to see if their symptoms get better.
- Keep your child away from smoky areas.
If these steps don't work, the doctor may suggest medicine. Medicines that may be used include:
- Acid reducers that decrease the amount of acid the stomach makes.
- H2 blockers, such as cimetidine (Tagamet) or famotidine (Pepcid). H2 blockers reduce the amount of acid in the stomach.
- Proton pump inhibitors, such as esomeprazole (Nexium), lansoprazole (Prevacid), and omeprazole (Prilosec).
Children with reflux rarely need surgery.
Related Information
Credits
Current as of: October 24, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 24, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.