Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Topic Contents
Pacemaker
Treatment Overview
A pacemaker is a small device. It sends out mild electrical signals that keep your heart beating normally. The signals are painless. It can help stop the dizziness, fainting, and shortness of breath caused by a slow or unsteady heartbeat.
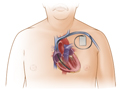
A pacemaker is powered by batteries. Most pacemakers are placed under the skin of your chest. They have thin wires, called leads. The leads pass through a vein into your heart.
A pacemaker can help restore a normal heart rate. It is used when certain problems have damaged the heart's electrical system, which normally keeps your heart beating steadily.
If you are worried about having a pacemaker, it may help if you learn about how the pacemaker helps your heart. Talk to your doctor about your concerns.
What To Expect
You may stay overnight in the hospital after having a pacemaker implanted and go home the next day. But sometimes, the surgery is done as an outpatient procedure, which means you do not need to stay overnight in the hospital.
You may be able to go back to work or your usual routine 1 to 2 weeks after surgery. But for at least a few weeks after the surgery, you should avoid vigorous physical activity that involves your upper body.
You'll need to use certain electric devices with caution. Some devices have a strong electromagnetic field. This field can keep your pacemaker from working right for a short time. These devices include things in your home, garage, or workplace. Check with your doctor about what you need to avoid and what you need to keep a short distance away from your pacemaker. Many household and office electronics don't affect your pacemaker.
Your doctor will check your pacemaker regularly. Your doctor may adjust it, if needed. In between checkups at your doctor's office, you may send information from your pacemaker to your doctor. Your doctor will give you instructions on how to do this.
Permanent pacemakers are powered by batteries. The batteries may last about 10 years. If the battery gets low, you will need to decide whether to have another surgery to replace the pacemaker.
Learn more
Why It Is Done
Your doctor might recommend that you get a pacemaker if:
- You have a problem with your heart rhythm that could be helped by a pacemaker.
- You have trouble doing everyday activities, or you can't do them at all.
Learn more
How Well It Works
Pacemakers stimulate the heart to speed up when it beats too slowly. They can also substitute for the natural pacemaker of the heart (SA node) or the heart tissue that regulates the beating of the ventricles (AV node).
Pacemakers can improve quality of life. For example, pacemakers can help people to return to normal, active lives.
Risks
There are several risks to getting a pacemaker. But risks vary for each person. And risks vary based on the type of pacemaker you get. Your doctor can help you understand your risk.
You will see your doctor regularly to check your pacemaker and make sure you don't have any problems.
During and soon after the procedure
Problems can happen during or soon after the procedure to implant a pacemaker. Examples of problems include the following:
- Pain, bleeding, or bruising may happen soon after the procedure.
- Blood clots may form in your arms, which cause a lot of swelling.
- A lung could collapse (pneumothorax). This happens if air builds up in the space between the lung and the chest wall. This problem may happen about 1 to 2 times out of a 100.footnote 1
- A tear in the heart could happen. Or a person might need emergency medicine or surgery.
After the procedure
Problems can also happen months or years after the pacemaker is implanted. These problems are related to the device or the leads. Most people do not have long-term issues with their pacemakers.
Problems include:
- Infection in your chest near the pacemaker. An infection might happen about 1 to 5 times out of 100. This means that about 95 to 99 times out of 100 there is no infection.footnote 1
- Device problems that need another procedure to fix them. For example, this might happen if a pacemaker lead breaks or a lead moves out of place.
Credits
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.